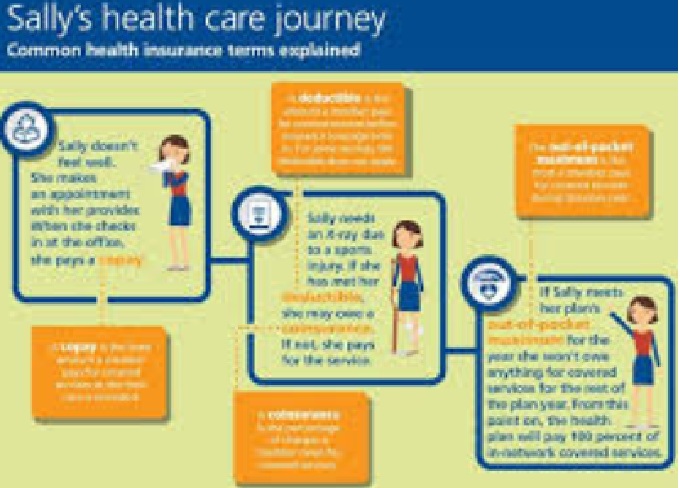
Health insurance is often described as a safety net that protects individuals and families from overwhelming medical expenses. Yet, for beginners, navigating the world of health insurance can feel like learning a new language. Policy documents are full of terms and phrases that may seem confusing or even intimidating. Without understanding these key terms, you might miss out on important benefits, choose the wrong plan, or end up paying more than expected.
This article breaks down the most common health insurance terms into simple, beginner-friendly explanations, helping you gain confidence in choosing and using your health insurance plan effectively.
Why Understanding Health Insurance Terms Matters
Before diving into the terminology, it’s important to understand why these terms matter.
-
Better decision-making – Knowing the language allows you to compare plans accurately and pick one that suits your budget and health needs.
-
Avoiding surprises – Misunderstanding terms like deductible or copayment can lead to unexpected out-of-pocket expenses.
-
Maximizing benefits – When you know how your policy works, you can use preventive care, wellness programs, and other covered services without confusion.
-
Financial security – Clarity helps you avoid paying unnecessary costs or missing claims.
Key Health Insurance Terms Explained
Below is a list of the most common health insurance terms, broken down with examples and easy-to-understand explanations.
1. Premium
Your premium is the amount you pay (usually monthly, quarterly, or annually) to keep your health insurance policy active. Think of it as a subscription fee.
-
Example: If your health insurance premium is $100 per month, you must pay that amount whether or not you use medical services.
Tip: Cheaper premiums often come with higher out-of-pocket costs, while higher premiums usually mean lower costs when you actually receive care.
2. Deductible
The deductible is the amount you must pay for healthcare services before your insurance company starts sharing the cost.
-
Example: If your deductible is $1,000, you pay the first $1,000 of your medical expenses in a year. After that, your insurance kicks in.
Tip: Plans with higher deductibles typically have lower premiums, making them suitable for healthy individuals who don’t expect frequent medical visits.
3. Copayment (Copay)
A copayment is a fixed amount you pay for a healthcare service, usually at the time of service.
-
Example: You might pay $20 for a doctor’s visit or $10 for a prescription, while your insurance covers the rest.
Tip: Copays do not usually count toward your deductible but do count toward your out-of-pocket maximum (explained later).
4. Coinsurance
Unlike a copay, coinsurance is not a fixed fee but a percentage of the cost of care.
-
Example: If your plan has 20% coinsurance and your medical bill is $1,000, you pay $200, and your insurance covers $800 (after meeting your deductible).
Tip: Coinsurance can significantly impact costs for expensive procedures, so check this percentage carefully.
5. Out-of-Pocket Maximum
The out-of-pocket maximum is the most you’ll have to pay for covered healthcare services in a policy year. Once you reach this limit, your insurance company pays 100% of the covered costs.
-
Example: If your out-of-pocket maximum is $6,000, once you’ve paid that much in deductibles, copays, and coinsurance, you won’t pay more for covered services that year.
Tip: This is a key term for protecting yourself from catastrophic medical bills.
6. Network
A network is a group of doctors, hospitals, pharmacies, and other healthcare providers that contract with your insurance company to provide services at discounted rates.
-
In-Network Providers: These doctors or hospitals have agreements with your insurer, which means lower costs for you.
-
Out-of-Network Providers: Using them may cost much more, and sometimes they are not covered at all.
Tip: Always check if your doctor or hospital is in your plan’s network.
7. Preauthorization (Prior Authorization)
Some services require preauthorization before your insurance company agrees to cover them. This means your doctor must get approval from your insurer before certain tests, procedures, or medications.
-
Example: An MRI might need preauthorization to ensure it’s medically necessary.
Tip: If you skip this step, your insurer might refuse to cover the cost.
8. Formulary
A formulary is the list of prescription drugs your insurance plan covers. These drugs are usually divided into tiers that determine your out-of-pocket costs.
-
Tier 1: Generic drugs (lowest cost).
-
Tier 2: Preferred brand-name drugs (moderate cost).
-
Tier 3 or higher: Non-preferred or specialty drugs (highest cost).
Tip: Always check if your medication is included in your plan’s formulary to avoid surprises.
9. Explanation of Benefits (EOB)
An EOB is a statement your insurer sends after you receive care. It is not a bill but an explanation of what was charged, what your insurance covered, and what you still owe.
-
Example: Your EOB might show your doctor charged $200, insurance covered $150, and you owe $50.
Tip: Always review EOBs to catch billing errors.
10. Claim
A claim is a request for payment submitted to the insurance company for healthcare services you received. Usually, the healthcare provider files this on your behalf.
-
Example: After a hospital visit, the hospital sends a claim to your insurer asking for payment.
Tip: Sometimes, if you visit an out-of-network provider, you might need to submit claims yourself.
11. Preventive Care
Most health insurance plans cover preventive care at no additional cost when you use in-network providers. This includes services like vaccinations, annual checkups, and screenings.
Tip: Preventive care is often covered without applying your deductible, meaning you don’t pay extra for it.
12. Pre-existing Condition
A pre-existing condition is a health issue you had before enrolling in a new insurance plan.
-
Example: Diabetes, asthma, or high blood pressure.
Tip: Many modern health insurance laws protect you from being denied coverage due to pre-existing conditions, but always check your plan’s rules.
13. HMO, PPO, EPO, and POS Plans
These acronyms describe different types of health insurance plans:
-
HMO (Health Maintenance Organization): Requires you to use in-network providers and get referrals for specialists. Lower cost, but less flexibility.
-
PPO (Preferred Provider Organization): More flexibility in choosing doctors, including out-of-network, but higher costs.
-
EPO (Exclusive Provider Organization): Like an HMO but usually doesn’t require referrals. No out-of-network coverage.
-
POS (Point of Service): Hybrid plan that combines features of HMO and PPO.
Tip: Your choice depends on whether you prioritize cost savings or flexibility.
14. Grace Period
The grace period is the extra time (usually 30 days) you have to pay your premium after the due date before your policy is canceled.
Tip: Missing payments beyond the grace period can result in losing coverage.
15. Lifetime Maximum
Some older insurance policies had a lifetime maximum, which capped the total amount the insurer would pay during your lifetime. Many modern plans have removed these caps due to regulations, but it’s worth checking.
16. Waiting Period
Some policies require a waiting period before certain benefits take effect.
-
Example: Maternity benefits might only be available after a 12-month waiting period.
Tip: Understand waiting periods before purchasing a plan to avoid disappointment.
17. Sub-limit
A sub-limit is a cap on specific expenses within your policy.
-
Example: Your plan might cover hospitalization but set a sub-limit of $500 per day for room rent.
Tip: Sub-limits can significantly reduce reimbursements, so read the fine print carefully.
18. Cashless Facility
In many countries, insurers partner with hospitals to offer a cashless facility. This means you don’t pay upfront for treatment—the insurer settles bills directly with the hospital.
Tip: Always check the list of network hospitals offering cashless treatment.
19. Exclusions
Exclusions are medical services or conditions your insurance does not cover.
-
Example: Cosmetic surgeries or dental procedures may be excluded.
Tip: Always read your policy’s exclusion list before signing up.
20. Rider (Add-on Cover)
A rider is an extra feature or benefit you can add to your base insurance policy, often for an additional cost.
-
Example: Critical illness rider, maternity rider, or accidental coverage rider.
Tip: Riders help customize your policy to fit your specific needs.
How These Terms Work Together (Example Scenario)
Imagine you buy a health insurance policy with:
-
Premium: $120/month
-
Deductible: $1,000
-
Coinsurance: 20%
-
Out-of-pocket maximum: $6,000
If you undergo surgery costing $10,000:
-
You first pay your $1,000 deductible.
-
Insurance covers 80% of the remaining $9,000 = $7,200.
-
You pay 20% of $9,000 = $1,800.
-
Your total cost = $2,800 (deductible + coinsurance).
If you had multiple procedures in the same year and reached the $6,000 out-of-pocket maximum, the insurer would cover all further expenses for the rest of the year.
Tips for Beginners Navigating Health Insurance
-
Make a glossary: Keep a personal list of terms and definitions for easy reference.
-
Compare carefully: Don’t just focus on premiums; look at deductibles, copays, coinsurance, and out-of-pocket maximums.
-
Check networks: Ensure your preferred doctors and hospitals are included.
-
Read exclusions: Know what isn’t covered to avoid surprises.
-
Use preventive care: Take advantage of free checkups and screenings.
Conclusion
Health insurance can seem overwhelming at first, but once you understand the key terms—like premium, deductible, copay, coinsurance, and network—the system becomes much clearer. These terms are the building blocks of every policy, and knowing them helps you make informed choices, avoid costly mistakes, and maximize the benefits available to you.
Whether you’re buying your first plan or simply trying to understand your current policy, learning these basics puts you in control of your health and financial security.